Meet Dr. Yokota
 A native Californian, Dr. Yokota graduated from the University of Southern California with a degree in Biological Sciences then received a dental degree from the University of the Pacific School of Dentistry in San Francisco, CA. For five years, Dr. Yokota practiced general dentistry before starting his endodontic residency at Indiana University School of Dentistry where he earned both an endodontic certificate and master’s degree. His training was focused on root canal therapy and endodontic microsurgery. In addition, Dr. Yokota was a clinical instructor and conducted early research on digital radiography which was published in the Journal of Endodontics. Afterwards, Dr. Yokota returned to San Jose to establish his endodontic practice in Willow Glen in 1993.
A native Californian, Dr. Yokota graduated from the University of Southern California with a degree in Biological Sciences then received a dental degree from the University of the Pacific School of Dentistry in San Francisco, CA. For five years, Dr. Yokota practiced general dentistry before starting his endodontic residency at Indiana University School of Dentistry where he earned both an endodontic certificate and master’s degree. His training was focused on root canal therapy and endodontic microsurgery. In addition, Dr. Yokota was a clinical instructor and conducted early research on digital radiography which was published in the Journal of Endodontics. Afterwards, Dr. Yokota returned to San Jose to establish his endodontic practice in Willow Glen in 1993.
Dr. Yokota is a long time member of the Santa Clara Dental Society, California Dental Association, American Dental Association, American Association of Endodontists, and Northern California Association of Endodontists. He is also a board certified Diplomate of the American Board of Endodontics, one of the few in the valley.
Dr. Yokota enjoys keeping up with the latest developments in endodontics. Each operatory is equipped with a surgical operating microscope and digital radiography. He takes several continuing education courses a year, constantly updating his knowledge. Outside the office, he enjoys the San Jose Sharks, cycling, and skiing with his wife and children.
Root Canal Therapy
Root Canal Therapy
What is a root canal?
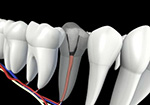 A root canal is one of the most common dental procedures performed, well over 14 million every year.
A root canal is one of the most common dental procedures performed, well over 14 million every year.
This simple treatment can save your natural teeth and prevent the need of dental implants or bridges.
At the center of your tooth is pulp. Pulp is a collection of blood vessels that helps to build the surrounding tooth. Infection of the pulp can be caused by trauma to the tooth, deep decay, cracks and chips, or repeated dental procedures. Symptoms of the infection can be identified as visible injury or swelling of the tooth, sensitivity to temperature or pain in the tooth and gums.
If you experience any of these symptoms, your dentist will most likely recommend non-surgical treatment to eliminate the diseased pulp. This injured pulp is removed and the root canal system is thoroughly cleaned and sealed. This therapy usually involves local anesthesia and may be completed in one or more visits depending on the treatment required. Success for this type of treatment occurs in about 90% of cases. If your tooth is not amenable to endodontic treatment or the chance of success is unfavorable, you will be informed at the time of consultation or when a complication becomes evident during or after treatment. We use local anesthesia to eliminate discomfort. In addition, we will provide nitrous oxide analgesia if indicated. You will be able to drive home after your treatment, and you probably will be comfortable returning to your normal routine.
What happens after treatment?
When your root canal therapy has been completed, a record of your treatment will be sent to your restorative dentist. You should contact their office for a follow-up restoration within a few weeks of completion at our office. Your restorative dentist will decide on what type of restoration is necessary to protect your tooth. It is rare for endodontic patients to experience complications after routine endodontic treatment or microsurgery. If a problem does occur, however, we are available at all times to respond. To prevent further decay, continue to practice good dental hygiene.
How much will it cost?
The cost associated with this procedure can vary depending on factors such as the severity of damage to the affected tooth and which tooth is affected. In general, endodontic treatment is much less expensive than tooth removal and replacement with an artificial tooth.
Endodontic Retreatment
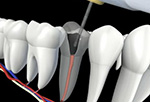 With the appropriate care, your teeth that have had endodontic treatment will last as long as other natural teeth.
With the appropriate care, your teeth that have had endodontic treatment will last as long as other natural teeth.
Yet, a tooth that has received treatment may fail to heal or pain may continue to exist. Sometimes, the pain may occur months or years after treatment. If so, Endodontic Retreatment may be needed.
Improper healing may be caused by:
- Curved or narrow canals were not treated during the initial treatment.
- Complicated canals went undetected during the initial treatment.
- The crown or restoration was not placed within the appropriate amount of time following the procedure.
- The crown or restoration did not prevent saliva from contaminating the inside of the tooth.
In some cases, new problems can influence a tooth that was successfully treated:
- New decay can expose a root canal filling material, causing infection.
- A cracked or loose filling or crown can expose the tooth to new infection.
Once retreatment has been selected as a solution to your problem, the doctors will reopen your tooth to gain access to the root canal filling material. This restorative material will be removed to enable access to the root canal. The doctors will now clean your canals and carefully examine the inside of the problematic tooth. Once cleaned, the doctors will fill and seal the canals and place a temporary filling in the tooth.
At this point, you will need to return to your dentist as soon as possible in order to have a new crown or restoration placed on the tooth to restore full functionality.
Apicoectomy
Apicoectomy
Why would I need Endodontic Surgery?
Generally, a root canal is all that is needed to save teeth with injured pulp from extraction. Occasionally, this non-surgical procedure will not be sufficient to heal the tooth and your endodontist will recommend surgery. Endodontic surgery can be used to locate fractures or hidden canals that do not appear on x-rays but still manifest pain in the tooth. Damaged root surfaces or the surrounding bone may also be treated with this procedure. The most common surgery used to save damaged teeth is an apicoectomy or root-end resection.
What is an Apicoectomy?
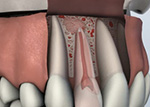 For this simple procedure an incision is made in the gum tissue to expose the bone and surrounding
inflamed tissue. The damaged tissue is removed along with the end of the root tip. A root-end filling is placed to prevent
reinfection of the root and the gum is sutured. The bone naturally heals around the root over a period of months restoring
full function.
For this simple procedure an incision is made in the gum tissue to expose the bone and surrounding
inflamed tissue. The damaged tissue is removed along with the end of the root tip. A root-end filling is placed to prevent
reinfection of the root and the gum is sutured. The bone naturally heals around the root over a period of months restoring
full function.
Following the procedure, there may be some discomfort or slight swelling while the incision heals. This is normal for any surgical procedure. To alleviate any discomfort, an appropriate pain medication will be recommended. If you have pain that does not respond to medication, please call our office.
Cracked Teeth
Cracked Teeth
Cracked teeth demonstrate many types of symptoms, including pain when chewing, temperature sensitivities, or even the release of biting pressure. It is also common for pain to come and go, making it difficult to diagnose the cause of discomfort.
Chewing can cause movement of the cracked pieces of your tooth, and the pulp within the tooth becomes irritated. At the same time, when biting pressure is released, the crack can close quickly, resulting in sharp pain. Eventually, the pulp will become damaged and tooth will consistently hurt, even when you are not chewing. It is possible that cracks can lead to infection of the pulp tissue, which can spread to the bone and gum surrounding the problematic tooth.
Types of Cracks
Craze lines
These are tiny cracks that only affect the outer enamel of the tooth. These cracks are more common in adults. These types of cracks are superficial and are usually of no concern.
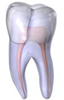 Fractured Cusp
Fractured Cusp
When a cusp becomes weakened, a fracture may result. The cusp may break off or be removed by a dentist. A fractured cusp rarely damages the pulp, so root canal is not necessary. Your dentist will usually restore the tooth with a full crown.
 Cracked Tooth
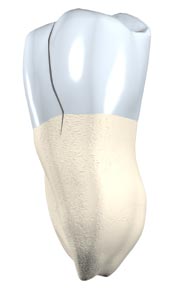
Cracked Tooth
This type of crack extends from the chewing surface of the tooth and vertically migrates towards the root. In some cases, the crack may extend below the gum line. It is possible for the crack to extend further into the root. Damage to the pulp is commonplace. In this case, root canal treatment is usually necessary. A cracked tooth that is not treated will worsen, resulting in the loss of the tooth. Therefore, early detection is essential.
 Split Tooth
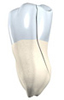
Split Tooth
A split tooth is usually the result of an untreated cracked tooth. It can be identified by a crack with distinct segments. This type of tooth can never be saved intact. Yet, the position and extent of the problem will dictate whether any portion of the tooth can be saved. Sometimes, endodontic retreatment by the doctors and restoration by your dentist can be used to save a portion of the tooth.
 Vertical Root Fracture
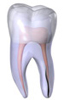
Vertical Root Fracture
A vertical root fracture begins at the root and extends towards the chewing surface of the tooth. Unfortunately, they show minimal symptoms and may go unnoticed. Treatment involves endodontic surgery if a portion of the tooth can be saved by removal of the fractured root. Otherwise the tooth will have to be extracted.
Traumatic Injuries
Traumatic Injuries
Dislodged Teeth
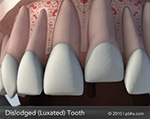 Injuries to the mouth can cause teeth to be pushed back into their sockets. Your endodontist or general dentist may reposition
and stabilize your tooth. Root canal treatment is usually started within a few weeks of the injury and a medication, such
as calcium hydroxide, will be placed inside the tooth. Eventually, a permanent root canal filling will be implanted.
Injuries to the mouth can cause teeth to be pushed back into their sockets. Your endodontist or general dentist may reposition
and stabilize your tooth. Root canal treatment is usually started within a few weeks of the injury and a medication, such
as calcium hydroxide, will be placed inside the tooth. Eventually, a permanent root canal filling will be implanted.
Sometimes a tooth may be pushed partially out of the socket. Again, your endodontist or general dentist may reposition and stabilize your tooth. If the pulp remains healthy, then no other treatment is necessary. Yet, if the pulp becomes damaged or infected, root canal treatment will be required.
Avulsed Teeth
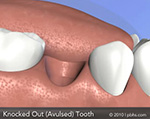 If an injury causes a tooth to be completely knocked out of your mouth, it is important that you are treated immediately!
If this happens to you, keep the tooth moist. If possible, put it back into the socket. A tooth can be saved if it remains
moist. You can even put the tooth in milk or a glass of water (add a pinch of salt.) Your Endodontist may start root canal
treatment based upon the stage of root development. The length of time the tooth was out of your mouth and the way the tooth
was stored, may influence the type of treatment you receive.
If an injury causes a tooth to be completely knocked out of your mouth, it is important that you are treated immediately!
If this happens to you, keep the tooth moist. If possible, put it back into the socket. A tooth can be saved if it remains
moist. You can even put the tooth in milk or a glass of water (add a pinch of salt.) Your Endodontist may start root canal
treatment based upon the stage of root development. The length of time the tooth was out of your mouth and the way the tooth
was stored, may influence the type of treatment you receive.
Injuries in children
An injured immature tooth may need one of the following procedures to improve the chances of saving the tooth:
Apexogenesis
This procedure encourages the root to continue development as the pulp is healed. Soft tissue is covered with medication to encourage growth. The tip of the root (apex) will continue to close as the child gets older. In turn, the walls of the root canal will thicken. If the pulp heals, no additional treatment will be necessary. The more mature the root becomes, the better the chance to save the tooth.
Apexification
In this case, the unhealthy pulp is removed. The doctors place medication into the root to help a hard tissue form near the root tip. This hardened tissue provides a barrier for the root canal filling. At this point, the root canal walls will not continue to develop, making the tooth susceptible to fractures. So it is important to have the tooth properly restored by your dentist.
Instructions
Before Endodontic Treatment
This procedure will be performed using local anesthesia. There are usually no restrictions after the procedure concerning driving or returning to work. A doctor is available for consultation at all times should a problem arise after your treatment.
Continue all medications for blood pressure, diabetes, thyroid problems and any other conditions as recommended by your physician. If there is a question, please call our office prior to your appointment.
Please eat a full breakfast or lunch as applicable.
If you have been advised by your physician or dentist to use antibiotic premedication because of mitral valve prolapse (MVP), heart murmur, hip, knee, cardiac or other prosthesis, or if you have rheumatic heart disease, please make sure you are on the appropriate antibiotic on the day of your appointment. If there is a question, please call our office prior to your appointment.
If you can take ibuprofen (Advil) or naproxen sodium (Aleve), it does help reduce inflammation when taken pre-operatively. We recommend 2 tablets of either medication 2-4 hours before endodontic therapy.
Please bring all referral information.
All patients under 18 must be accompanied by parents or guardian.
If you have any questions, please call our office at 408-978-3636
Home Care Instructions
Endodontic treatment will be performed using local anesthesia. There are usually no restrictions after the procedure concerning driving or returning to work. A doctor is available for consultation at all times should a problem arise after your treatment.
Continue all medications for blood pressure, diabetes, thyroid problems and any other conditions as recommended by your physician. If there is a question, please call our office prior to your appointment.
Please eat a full breakfast or lunch as applicable.
If you have been advised by your physician or dentist to use antibiotic premedication because of mitral valve prolapse (MVP), heart murmur, hip, knee, cardiac or other prosthesis, or if you have rheumatic heart disease, please make sure you are on the appropriate antibiotic on the day of your appointment. If there is a question, please call our office prior to your appointment.
If you can take ibuprofen (Advil) or naproxen sodium (Aleve), it does help reduce inflammation when taken pre-operatively. We recommend 2 tablets of either medication 2-4 hours before endodontic therapy.
Please bring all referral information.
All patients under 18 must be accompanied by parents or guardian.
If you have any questions, please call our office at 408-978-3636
After Completion of Endodontic Treatment
Endodontic treatment has now been completed.The root canal system has been permanently sealed. However, the outer surface is sealed with a temporary restoration. A follow-up restoration must be placed to protect your tooth against fracture and decay. Please telephone your general dentist for an appointment, and our office will send a complete report of treatment.
Your tooth is more prone to fracture immediately after endodontic treatment. You should chew on the other side until your general dentist has placed a core build-up and a protective restoration, usually a crown. If your tooth’s strength is seriously compromised, your endodontist or restorative dentist may place a post and core build-up inside the tooth. Your general dentist and endodontist will determine the appropriate restoration to best protect your tooth.
Are There Any Potential Problems After Treatment?
- Lower teeth and nerve injury. There is a slight possibility that nerve injury can occur during root canal surgery to the lower posterior teeth. Your endodontist is trained to assess this possibility prior to treatment and will advise you accordingly. For lower posterior teeth, the root tips may be near a nerve that supplies feeling to the lip, chin and gums. Your endodontist is trained to design your surgery to minimize the chances of damaging this nerve. Rarely, this nerve can become irritated during the process of surgery. In these cases, when the local anesthesia wears off, you may experience tingling, altered sensation or, in rare cases a complete lack of feeling in the affected tissues. Should this occur, it is usually temporary and will resolve over a period of days, weeks or months. In rare cases, these changes can be permanent and/or painful.
- Upper teeth and sinus communication. The upper teeth are situated near your sinuses, and root canal surgery can result in a communication between your mouth and the adjacent sinus. Should this complication occur, it will usually heal spontaneously. We will give you special instructions if this is apparent at the time of surgery. We prefer that you don’t blow your nose for two to three days after surgery. If you have to sneeze, you should sneeze with an open mouth into a tissue. You should not create any pressure in the sinus area. If you sense a complication after surgery, please contact us.
- Post-operative infections.Post-operative infections occasionally occur. This usually requires just an office visit and examination. Many times placing you on an antibiotic for one week will take care of the infection Occasionally, other follow-up procedures will be needed.
If you have any questions, please call our office at 408-978-3636
Before Surgery
In order to optimize treatment, and reduce swelling and discomfort, please follow these instructions prior to your surgery:
Avoid taking aspirin or any non-steroidal anti-flammatory drugs. ie; Advil, Ibuprofen, Motrin Aleve, Dolobid, or St. John's Worth or Fish Oil etc. 3-5 days prior to surgery.
If these medications or any other anticoagulants have been prescribed to you by your physician, advise us at the time of your consultation so we may discuss this with your MD.
Remember to have your regularly scheduled meals and wear loose and comfortable clothing.
DO NOT drink caffeinated drinks the day of the surgery.
DO NOT drink alcoholic beverages 2 days prior to surgery and 4 days after your surgery. Alcohol can cause excess bleeding and swelling and pain.
Take all prescribed medications as directed, unless you have been told otherwise. DO NOT drive or operate machinery while under the influence of prescription pain medication, ie, narcotics.
After Surgical Care
Take medication as directed. START BEFORE ANESTHESIA WEARS OFF. It will be more effective in minimizing post –operative discomfort.
- In order to keep possible swelling to a minimum, the use of an ice pack on the face over the surgical area is recommended. The ice pack should be used - 20 minutes on, 20 minutes off for the first 6 hours following surgery.
- You may lie in bed to rest however, your back must be elevated to avoid further swelling.
- In order to prevent tearing of the sutures and not retard healing, DO NOT RAISE YOUR LIP TO LOOK AT THE TREATED AREA.
- Mild oozing of blood, some swelling, mild discomfort and/or skin discoloration may be experienced. This will be temporary. If a temperature or excess bleeding should develop, call our office immediately.
- Avoid hot liquids and eat only soft foods for the first 48 hours. Use your own judgment after this period but avoid hard or chewy foods until your next visit. We recommend a cold liquid diet for the remaining day of surgery.
- No strenuous exercise should be performed for 3 days following surgery
- No smoking for at least 24 hours after surgery.
- Do not brush your teeth near the operated area until your follow up appointment; this will usually be a week post surgery. Brush your teeth in the rest of the mouth.
- Starting the day after surgery, lightly rinse your mouth with warm salt water. Do this following each meal and before bedtime.
- Get plenty of rest and insure normal intake of food, especially liquids such as fruit juices, soups and milk.
- We will see you in one week to evaluate healing and to remove sutures (if applicable). Should any difficulties arise in the meantime, please do not hesitate to call our office at any time - day, night or weekend.
- Continue taking any prescription drugs as directed.
- In some cases a biopsy of the infected tissue might be necessary. This will be sent to an oral pathology lab for examination. Any additional fee for this service will be billed directly to you by the laboratory.
Follow Up Care
- Arrangements to see your general dentist need to be made as soon as possible to have your tooth permanently restored.
- In six months you will be receiving a postcard from us for a follow up exam to evaluate the progress of healing.
- Please call us to make an appointment when you have received this postcard.
First Visit
First Visit
Your initial appointment will consist of a consultation explaining your diagnosis and treatment options. Often, treatment can be done the same day as the consultation as many first visits are emergencies. However, a complex medical history or treatment plan will require an evaluation and a second appointment to provide treatment on another day.
Please assist us by providing the following information at the time of your consultation:
- Your referral slip and any X-rays if applicable.
- A list of medications you are presently taking.
- If you have medical or dental insurance, bring the necessary completed forms. This will save time and allow us to help you process any claims.
IMPORTANT: A parent or guardian must accompany all patients under 18 at the consultation visit.
Please alert the office if you have a medical condition that may be of concern prior to surgery (i.e. diabetes, high blood pressure, artificial heart valves and joints, rheumatic fever, etc.) or if you are on any medication (i.e. heart medications, aspirin, anticoagulant therapy, etc.) or require medication prior to dental cleanings (i.e antibiotics, for pre-med.)
X-Rays
If your previous dentist has taken recent x-rays (within 6-months), you may request that they forward them to our office. If there is not enough time, please pick them up and bring them to our office. If additional films are necessary, they can be taken at our facility.
Scheduling
Scheduling
Our office is open Monday through Thursday from 8:30 AM until 5:00 PM and Friday by appointment only.
We will schedule your appointment as promptly as possible. If you have pain or an emergency situation, every attempt will be made to see you that day.
We try our best to stay on schedule to minimize your waiting. Due to the fact that Dr. Yokota sees many emergencies, various circumstances may lengthen the time allocated for a procedure. Unscheduled appointments can cause delays. We appreciate your understanding and patience.
Please call us at 408-978-3636 with any questions or to schedule an appointment.
Patient Forms
Please visit our website on a pc to download the patient history and registration form, print to fill out and bring to your next visit.
Note: These forms do not schedule an appointment; Please call us at 408-978-3636 to make an appointment.
It is not necessary to fill out a health history form for every visit, but please inform us of any changes since your last visit.
Contact Us
Eric T. Yokota, DDS, MSD
1688 Willow St., Suite E
San Jose, CA 95125
Phone: 408-978-3636
Fax: 408-445-0320
Navigate arrows to left then click on "Get Directions" in address label
